News / Press Releases
Stay updated with all that is happening at CH-F!
Community Hospital - Fairfax Expands Access to Mental Health Care with Addition of Telehealth Psychiatrrict Dr. Farzan Fatemi
6/1/2026 – Community Hospital – Fairfax is pleased to announce the addition of psychiatrist Dr. Farzan Fatemi, who will begin offering telehealth appointments on June 10, 2026, through our Outpatient Specialty Clinic. Dr. Fatemi will provide virtual visits on the second Wednesday of each month, giving patients convenient access to high‑quality psychiatric care without the need for long travel.
This service directly addresses one of the top priorities identified in our Community Health Needs Assessment, which highlighted psychiatric and behavioral health care as a significant need in our community. By expanding telemedicine options, Community Hospital – Fairfax remains committed to reducing barriers and supporting the well‑being of our community.
Dr. Fatemi will see adult patients ages 18 and older. Pediatric patients will not be accepted at this time. A referral from a primary care provider is required before appointments can be scheduled.
Dr. Fatemi currently practices psychiatry in Minneapolis, Minnesota, and has been board certified in psychiatry and neurology since 2024. He completed his undergraduate studies in mathematics and biology at Northwestern University, earned his medical degree from the University of Minnesota, and completed residency training through the Hennepin‑Regions Psychiatry Training Program.
Dr. Fleming will continue seeing patients twice monthly on Thursdays. Patients who wish to transition their care to Dr. Fatemi may do so through a primary care referral that includes a note indicating the patient’s preference
.
To learn more, please contact the Outpatient Clinic at (660) 686‑2335.

Dr. Farzan Fatemi

Dr. Burke calls into the system from a remote location to demonstrate the capabilities of the new TeleDigm system. The technology allows providers to assess patients using state-of-the-art monitoring and high-quality video..
Community Hospital–Fairfax Launches Advanced TeleStroke Program in Partnership with Nebraska Medicine
5/26/2026 – Community Hospital–Fairfax (CH‑F) has announced the launch of a state‑of‑the‑art TeleStroke program, made possible through a collaboration with Nebraska Medicine TeleStroke Neurology Services. This new technology brings rapid, specialized stroke care directly to the CH‑F Emergency Department, ensuring that patients in rural communities can receive expert neurological evaluation without leaving our community.
When a patient arrives with possible stroke symptoms, time is everything. The Emergency Department team immediately begins assessment and imaging, including a CT scan. Simultaneously, nursing staff enter critical patient information into the TeleDoc system. Once submitted, the team contacts the TeleStroke center at Nebraska Medicine to provide an initial report. Within moments, a stroke neurologist joins the patient’s room remotely through the Teledigm camera system.
The system is designed for seamless use. Staff do not need to operate or activate the camera. The neurologist can control the equipment remotely, allowing them to conduct a real‑time neurological exam from miles away. Using high‑resolution camera technology, the neurologist evaluates the patient’s speech, movement, responses, and pupils, while also reviewing bedside monitors and communicating directly with the care team. Each room is equipped with a digital stethoscope, enabling the neurologist to listen to heart and lung sounds in real time.
One of the most significant advantages of the TeleStroke program is the neurologist’s immediate access to CT imaging. Nebraska Medicine specialists can review radiology images instantly, allowing for rapid interpretation and timely treatment recommendations during these critical moments.
Following the assessment, the neurologist collaborates with the Emergency Department provider to determine the best course of action. This may include administering TNKase, a clot‑busting medication used to treat ischemic strokes. If a hemorrhagic stroke is identified, the neurologist provides immediate guidance for stabilization and next steps. When a higher level of care is required, the neurologist assists with coordinating transfer to Nebraska Medicine or another appropriate facility. In many cases, the same neurologist who evaluates the patient via camera at CH-F will continue caring for them after transfer, providing valuable continuity for patients and families.
To support consistent, evidence‑based care, the TeleStroke team has developed a standardized stroke algorithm in partnership with Nebraska Medicine. CH‑F will closely monitor “Door In, Door Out” times, aiming for transfers within 90 minutes when advanced stroke care is needed. The hospital is also working closely with Atchison Holt Ambulance District to ensure efficient patient transfers.
This program represents months of collaboration, planning, and testing among Community Hospital–Fairfax, Nebraska Medicine, TeleDoc, and Teledigm. Key contributors include Ashlee Driskell and Samantha Grist from CH‑F; Dr. Kelly‑Ann Patrice and Denise Gorski from Nebraska Medicine Neurology; and Erin Williams and Erin Leifer from TeleDoc. Additionally, Dr. Burke can access the system remotely to support Emergency Department providers during urgent situations.
For rural communities, access to specialized stroke care can be life‑changing. The TeleStroke program enhances speed, coordination, and continuity of care—bringing expert neurological evaluation directly to patients when every second counts.
Senior Life Solutions Celebrates a Decade in Bloom with 10th Anniversary Garden Party Open House











5/13/2026 – Over the past 10 years, Community Hospital-Fairfax’s Senior Life Solutions program has positively touched the lives of 183 patients who needed a mental and emotional health boost. On May 13, 2026, Senior Life Solutions hosted an open house garden party to celebrate 10 years of providing care to seniors in our community.
Program Director, Gail Heitman, RN, had this to say, “It is my privilege to work with our fantastic team at Community Hospital-Fairfax — Karia Browning, OPC; Sarah Watkins, LPC; Cheyann Wheeler, LMSW and Stacey Stillwell, LPN
As we celebrate our 10th Anniversary, I think I can speak for the entire team when I say we love what we do, and it is so rewarding to see our patients thrive mentally. Depression and anxiety stalk many people in our world today, due to a variety of reasons. It is comforting to know that right here at home, Community Hospital – Fairfax’s Senior Life Solutions offers help for those in need.
I have been a nurse for over 42 years in Holt and Atchison counties. When I was asked 10 years ago to be the program director for Senior Life Solutions, I could think of so many different patients that had crossed my path throughout the years that would have benefitted greatly from this program, but there were no programs like it at the time.
In honor of those patients and family members, and with encouragement from my daughter, who is a nurse, I said, “I’ll give it a whirl!”
I have never looked back! Ten years have flown by! I consider this role a calling rather than a job, and I am so blessed to be a part of it!
Anyone can refer to our program, including family members, physicians, pastors, hospital employees, and community members. Patients can also refer themselves! Once referred, we will screen them to ensure that they meet the qualification for our program.
Our phone number is 660 686 2319. Give us a call today!”
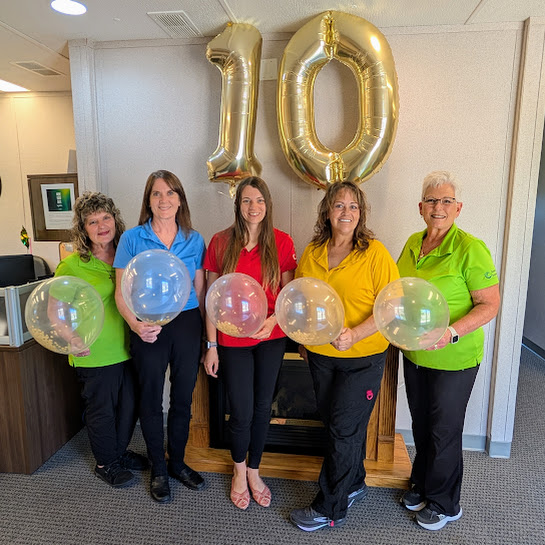
Karia Browning, OPC; Sarah Watkins, LPC; Cheyann Wheeler, LMSW, and Stacey Stillwell, LPN

Community Hospital – Fairfax OB Nursing Team
Front row: Holly Gray RN, Kim Giles RN, Michelle Bollinger RN, Back row: Ashlee Driskell RN – Director of OB Nursing, Kelsi Oberhauser RN
Community Hospital - Fairfax strengthens Obstetric and Neonatal Care for high-risk situations
4/22/2026 – Rural hospitals across the country are shuttering obstetrics and labor and delivery services due to financial constraints and provider shortages. In Missouri, 42% of counties are classified as OB deserts. Meanwhile, the OB team at Community Hospital – Fairfax is making big strides to raise the bar for rural maternal and neonatal care in our community and across the state.
The OB team at CH-F is a part of the Missouri Perinatal Quality Collaborative (PQC), a statewide program focused on bringing hospitals together to develop evidence-based practices, track results, and continuously improve outcomes for mothers and babies.
“For CH-F, this means we are aligning ourselves with the highest state and national standards for obstetrics and neonatal care. We have been focusing specifically on two initiatives: obstetric hemorrhage, and the maternal-infant dyad affected by substance use disorder. We are using standardized guidelines, education, and data tracking to ensure we are prepared for emergencies and ready to provide compassionate, consistent care to both mothers and babies,” Director of Nursing, Ashlee Driskell, said.
CH-F’s work in obstetric hemorrhage has been ongoing since 2023. The OB team implemented use of an obstetrical hemorrhage cart which enables them to measure blood loss in real time to determine if another intervention is needed. One of two interventions, the JADA system, is housed in the cart. JADA utilizes low-level vacuum to induce a contraction and restrict blood flow.
The second area of focus for CH-F is the maternal-infant dyad affected by substance use disorder. This initiative includes more extensive screening and assessment for newborns, a protocol that prioritizes non-pharmacological care, and the implementation of the eat, sleep, and console model of care which prioritizes a newborn’s ability to perform basic functions over medical interventions. This approach often decreases the need for transfer and keeps newborns with their mothers whenever it is safe to do so.
“Our protocol is to prioritize non-pharmacologic care first. That means supporting bonding, decreased stimulation, encouraging skin-to-skin, and creating a calm environment for both mother and baby. This initiative is about treating mom and baby as one unit because what affects one, affects the other. At the end of the day, this initiative is about meeting families where they are, reducing stigma, and providing compassionate, supportive care. These are our people. Our neighbors. Our families. This work is about making sure moms and babies are safe, supported, and cared for close to home,” OB Nurse, Michelle Bollinger said.

Community Hospital - Fairfax Welcomes Lorraine Dodson, MD, FACOG as Specialist Provider for Gynecology Clinic and Gynecological Surgeries
4/1/2026 – Community Hospital – Fairfax is proud to announce a partnership with Mosaic Medical Center – Maryville and Lorraine Dodson, MD, FACOG to provide a gynecology specialty clinic and gynecological surgery services.
Dr. Dodson has cared for women in her OB/GYN practice for over 30 years. Dr. Dodson earned her bachelor’s degree in chemical biology from Rhodes College in Memphis, TN. She attended the University of Missouri – Columbia where she graduated cum laude with her medical degree as well as completed her residency.
“I’ve always enjoyed practicing in a small community where I can really get to know my patients and their families,” says Dr. Dodson
Dr. Dodson enjoys gardening, hiking, running and spending time with her numerous dogs, cats and horses. She and her husband, also a physician, have three grown children.
“We are excited to bring Dr. Dodson and her experience in gynecological surgeries to CH-F. We recognize that these are services that the women of our community are traveling to receive so we are looking forward to bringing them back, close to home, for our patients,” CEO, Ann Schlueter, commented.
Dr. Dodson’s first clinic day at Community Hospital – Fairfax will be April 17, 2026. Please call your primary care provider for a referral and to schedule an appointment.
Community Hospital - Fairfax named a Top 100 Critical Access Hospital by The Chartis Center for Rural Health for Second Year; Awarded Two Chartis Performance Leadership Awards


2/23/2026- Community Hospital – Fairfax today announced it has been recognized as a 2026 Top 100 Critical Access Hospital by The Chartis Center for Rural Health. The Top 100 awards program celebrates outstanding performance annually among the nation’s rural hospitals based on the results of the Chartis Rural Hospital Performance INDEX®.
“We know how fortunate we are to serve this community, who trusts us with their care and supports the work that we do. This hospital belongs to the people we serve who deserve timely, effective, and compassionate care. It is our honor to be able to provide it,” CEO of Community Hospital – Fairfax, Ann Schlueter said.
“The delivery of care within rural communities is perhaps more complex today than at any point in recent memory. This year’s Top 100 Critical Access Hospitals have emerged as true leaders – committed to their mission through a powerful combination of resilience, dedication and innovation,” said Michael Topchik, Executive Director of The Chartis Center for Rural Health. “We’re delighted to recognize this year’s winners and celebrate their Top 100 status.”
Now in its 16th year, the INDEX is the industry’s most comprehensive and objective assessment of rural hospital performance. Leveraging publicly available data, the INDEX is utilized nationwide by rural hospitals, health systems with rural affiliates, hospital associations, and state offices of rural health to measure and monitor performance across a variety of areas impacting hospital operations, quality, patient perspective and finance.
In addition to being named a Chartis Top 100 Critical Access Hospital, Community Hospital Fairfax also received two Chartis Performance Leadership Awards in the categories of Quality and Patient Perspective. Compiled by The Chartis Center for Rural Health, the Performance Leadership Awards program recognizes top quartile performance (i.e., 75th percentile or above) among rural hospitals in Quality, Outcomes, and/or Patient Perspective.
“The areas of quality, outcomes, and patient perspective are cornerstones of healthcare delivery across rural America, and this year’s Performance Leadership Award recipients are establishing a standard of excellence for their rural peers to follow,” said Michael Topchik, Executive Director, Chartis Center for Rural Health. “We are delighted to shine a spotlight on such strong performance and honor the achievement of these hospitals.”
A Note from Ann's Desk
If you follow Community Hospital-Fairfax on social media, you will see a new tagline, “Medicine – The way it was meant to be.” In a world where “community” has become increasingly distant, in the halls of our hospital and clinics, we want you to feel at home. Medicine is science, but it needs relationships. Providing care and living life with you, well, we think that is just how medicine is supposed to be.
Community Hospital - Fairfax Honored with Missouri Hospital Association's 2025 Aim For Excellence Award

Photo caption: Craig Thompson, P.T., FACHE, CEO of Golden Valley Memorial Healthcare in Clinton, Mo., and 2025 MHA Board Chair (left), and Jon D. Doolittle, MHA President and CEO (right), present a 2025 Aim For Excellence Award to Heather Olson, R.N., Director of Primary Care Services at Community Hospital – Fairfax.

11/10/2025 – JEFFERSON CITY, Mo. — Community Hospital – Fairfax has been honored with the Missouri Hospital Association’s Aim for Excellence Award. Established in 2016, the Aim for Excellence Award recognizes hospital innovation that improves patient outcomes. The award was presented Nov. 5 at MHA’s 103rd Annual Convention in St. Charles, Mo.
“In the northwest Missouri communities around Fairfax, only 20% of Medicare beneficiaries were taking advantage of the program’s annual wellness visit,” said Jon D. Doolittle, MHA President and CEO. “What started as a program to improve engagement and increase participation has grown into a window to understand and address the drivers of good health.”
Community Hospital - Fairfax Voted Best of Midwest: Received Gold in four sub-categories, and a silver.

7/9/2025 – Community Hospital – Fairfax announced it was voted Best of Midwest in the sub-categories of, Best Hospital, Best Customer Service, Best Orthopedic Surgeon, and Best Medical Facility for Family Medicine Clinics. Physical Therapy received a silver medal for Best Physical Therapist.
Regional Media Inc out of Maryville opened nominations for its first ever Best of Midwest contest in March and opened voting to the community in April to promote economic growth and recognition for businesses in the region.
“What an honor it is to serve our community and hear their voices through the Best of Midwest awards. We are grateful to our community for voting for us. Receiving these awards in addition to being listed among the Chartis Top 100 Critical Access Hospitals in the nation has made this a very special 75th Anniversary year for Community Hospital – Fairfax,” CEO, Julie Jones, said.
Jones credits the staff, board of directors, and leadership of the organization for years of strategic planning and tremendous work.
“The recognition we are receiving is a culmination of years of continuous process improvement and dedication from our staff, board, and leadership team. Our efforts to update Radiology, increase quality standards and processes, deliver an outstanding customer experience and provide services that fill community needs have all contributed to the hospital and level of care you see today,” Jones said.
Community Hospital – Fairfax Family Medicine Clinics were voted Best Medical Facility.
Julie Jones had this to say, “Since its inception in 2016, our Family Medicine Clinics have dedicated their efforts to increasing access to primary care, disease prevention, and optimal wellness. We continue to adapt our care to better serve the community’s ever-changing primary care needs.”
After launching a new Orthopedic and Orthopedic Surgery Program in January through a partnership with Dr. John Weitlich, Community Hospital – Fairfax was honored to the receive Best Orthopedic Surgeon. Dr. Weitlich’s outpatient clinic added an additional day of service in July to accommodate the growing program.
“To be voted Best Orthopedic Surgeon after such a short time speaks volumes about Dr. Weitlich and the team we have at CH-F. Nearly every department has been involved in this expansion, and they have done outstanding work to make this program successful,” Julie Jones said.
Julie Jones to Retire as Community Hospital - Fairfax CEO, Ann Schlueter named Successor
6/9/2025 – In March 2025, Julie Jones announced her retirement as the CEO of Community Hospital – Fairfax (CH – F), effective September 30, 2025.
Julie was named CEO on January 1, 2019. She previously served as the Chief Nursing Officer of CH-F beginning in 2015. With Julie’s guidance the Board of Directors, medical staff, and employees developed and implemented a new mission, vision, and values to set the organization’s direction.
Over the last 6.5 years, Julie has led the hospital team in installing a wide-bore MRI, replacing the x-ray equipment, CT scanner, ultrasound equipment, and upgrading the surgery area to bring orthopedic surgery to our community. Additionally, an Advanced Wound Care program was started in 2021. Dr. Mina Massey joined the medical staff in 2023 to expand access to primary care in CH-F’s Family Medicine Clinics. The organization received a 5-star CMS patient satisfaction rating, and most recently was named a Chartis Top 100 Critical Access Hospital.
On Wednesday, June 4, 2025, the Board of Directors appointed Ann Schlueter, COO, as the new CEO of Community Hospital – Fairfax, effective October 1, 2025.
Ann Schlueter, MBA, has been part of the CH – F team since 2008, serving in various capacities and most recently as Chief Operating Officer. Ann is passionate about rural healthcare and CH – F’s mission to provide high quality and accessible healthcare close to home. Her dedication to quality and expertise in hospital processes has been instrumental in CH – F’s DNV-GL accreditation and ISO 9001 certification.
Ann looks forward to serving CH – F in a new capacity as the organization continues to care for the communities of Northwest Missouri. Ann resides in rural Atchison County with her husband Matt and three children, Aaron, Lizzie, and Josh.
“I have been honored to work with Julie and watch the impact she’s had during my time at Community Hospital – Fairfax. I am equally enthusiastic about working with Ann Schlueter as the new CEO. Ann has a strong commitment to quality and patient satisfaction, and I am confident that under her leadership, Community Hospital – Fairfax will continue to thrive,” Board Chairman Tim Umbarger said.

Community Hospital - Fairfax Recognized by Chartis as a Top 100 Critical Access Hospital
2/2025 – Community Hospital – Fairfax in Fairfax, Missouri today announced it has been named among the 2025 Top 100 Critical Access Hospitals by The Chartis Center for Rural Health. Chartis’ annual Top 100 award program honors outstanding performance among the nation’s rural hospitals based on the results of the Chartis Rural Hospital Performance INDEX®.
“We are excited to share this news with our supportive community,” said Julie Jones, Chief Executive Officer for Community Hospital – Fairfax. “To be listed among Chartis’ Top 100 Critical Access Hospitals reflects our organization’s dedication to our core values: Excellence, Teamwork, Integrity, and Service. We have taken important steps over the last five years to demonstrate our commitment to quality, patient satisfaction, and patient safety through our DNV-GL and ISO 9001 Accreditation. It is an honor for our entire team, once again, to be recognized for our progress.”
“The Top 100 Critical Access Hospitals award program elevates the very best performers and helps create a roadmap for those seeking to improve financial and operational performance while continuing to care for the communities they serve,” said Michael Topchik, Executive Director, The Chartis Center for Rural Health. “This is our 15th year recognizing the Top 100 Critical Access Hospitals and we’re thrilled to be able to celebrate this milestone with this year’s winners.”
The INDEX is the industry’s most comprehensive and objective assessment of rural hospital performance. Leveraging publicly available data, the INDEX is utilized nationwide by rural hospitals, health systems with rural affiliates, hospital associations, and state offices of rural health to measure and monitor performance across a variety of areas impacting hospital operations and finance.
To view the complete list of awardees, visit https://www.chartis.com/top-performing-rural-hospitals


Community Hospital - Fairfax welcomes John Weitlich M.D. to expand Orthopedic Program
Community Hospital – Fairfax is excited to introduce Dr. John Weitlich, is a Board-Certified orthopedic surgeon. Dr. Weitlich brings his expertise in general orthopedics and orthopedic trauma, specializing in the management of fractures and providing both operative and non-operative care for conditions such as thumb arthritis, wrist arthritis, knee arthritis, and pediatric fractures.
Growing up in a small, rural community himself, Dr. Weitlich has a deep understanding of the unique healthcare needs of rural residents. His personal connection to rural life fuels his dedication to delivering high-quality orthopedic care to our community.
Dr. Weitlich’s medical journey began with an undergraduate degree in biology from Benedictine College in Atchison, Kansas, where he also excelled in football and track. He earned his medical degree from the University of Kansas School of Medicine and completed his orthopedic residency at the University of Missouri. His passion for orthopedic surgery was ignited while working as a certified nursing assistant during college, inspired by shadowing Dr. Brett Miller.
In addition to his professional expertise, Dr. Weitlich is excited to introduce a total joint replacement program, beginning with total knee replacements, at Community Hospital Fairfax. This program will enhance our orthopedic services and provide advanced care options for our patients.
Outside of his professional life, Dr. Weitlich enjoys spending time outdoors, playing golf, and playing the guitar. He cherishes moments with his family, especially his wife and two daughters, and looks forward to contributing to the well-being of our rural community.
Join us in welcoming Dr. Weitlich to Community Hospital – Fairfax, where his commitment to our community’s health and his expertise in orthopedic care will make a significant impact on the lives of our patients.
Clarkson College and Community Hospital - Fairfax Continue Partnership to Build Healthcare Workforce
Contact: Kristin Camp
Communications Administrator
402-552-6476, CampKristin@ClarksonCollege.edu
Clarkson College and Community Hospital – Fairfax Continue Partnership to Build Healthcare Workforce
Fairfax Community Hospital employees, their spouses and dependents receive scholarships
Omaha, Neb.: The longtime partnership between Clarkson College and Community Hospital – Fairfax continues to strengthen as the institutions work together to build a highly skilled and compassionate healthcare workforce. The partnership offers Community Hospital – Fairfax employees as well as their spouses and dependent children substantial scholarships and preferred application status.
Community Hospital – Fairfax is a critical access hospital that provides 24-hour emergency services, diagnostic laboratory services, radiology services, and physical, occupational, and speech therapies to residents located in and around Fairfax, Missouri. Its facilities serve as the primary health care provider for residents of Atchison and Holt Counties, as well as some of Nodaway County.
In her remarks to attendees of Community Hospital’s annual Gala Dinner and Show on March 16, Julie Jones, CEO of Community Hospital – Fairfax, thanked Clarkson College for their sponsorship of the event. Mrs. Jones, a member of the Clarkson College Board of Directors, stated, “The importance of quality healthcare education is vital to rural, independent hospitals. We are pleased to partner with Clarkson College to provide scholarships to our employees and their family members. Our community is ultimately made stronger through this commitment.”
Dr. Andreia Nebel, President and CEO of Clarkson College acknowledged the partnership, saying, “by taking advantage of these scholarships, students may earn a quality healthcare education and pursue professional goals with reduced financial burden.”
The partnership offers Community Hospital – Fairfax employees, as well as their spouses and dependent children ages 23 and younger, substantial scholarships (example: approximately $32,000 over four years for a bachelor’s degree) at Clarkson College. All applicants who meet admissions qualifications and are seeking enrollment in online programs will be accepted. Preference will be given to applicants enrolling in on-campus programs through additional points on their application. Participants are also eligible to apply for Clarkson College academic scholarships and financial aid, and graduates will have the opportunity to gain salary and advancement potential at Community Hospital – Fairfax.
The partnership allows employees and their family members to pursue advanced education options in critical areas such as nursing. Clarkson College offers opportunities including Registered Nurse (RN) to Bachelor of Science in Nursing (BSN), traditional BSN, Master of Science in Nursing (MSN) and Doctor of Nursing Practice (DNP), as well as certificate and Nurse Anesthesia options. They can also explore healthcare education options in Physical Therapist Assistant, Radiography and Medical Imaging, Psychology, Healthcare Business, General Education, Health Information Management, Community Health, and Education and Leadership.
Learn more at ClarksonCollege.edu/Fairfax-Community-Hospital.


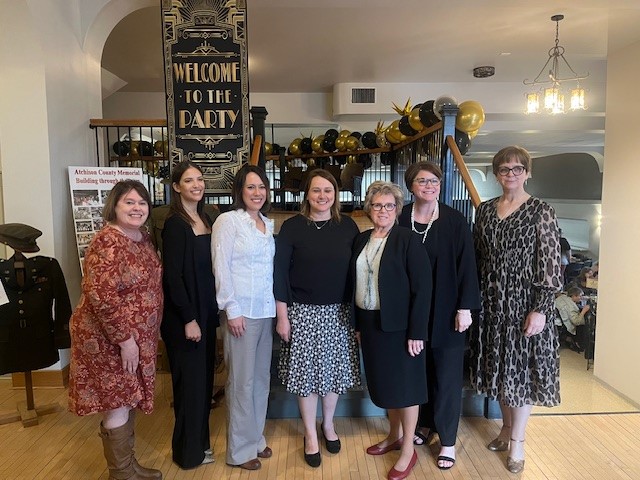
Clarkson College Sponsors Hospital Gala and Show
In attendance at the Community Hospital – Fairfax Gala March 16, 2024 were representatives of Clarkson College, pictured with hospital CEO, Julie Jones. From left: Lori Jerina, Ale Denton, Jessica Wissink, Clarkson College President Dr. Andreia Nebel, Ms. Jones, Jina Paul, and Kristin Camp.
Clarkson College is a private, non-profit college in Omaha, Neb. offering certificate, and degree opportunities in the fields of Nursing, Healthcare Business, Physical Therapist Assistant, Radiography, Medical Imaging, Imaging Informatics, Community Health, Healthcare Education and Leadership, Psychology and Community Advancement. The College is nationally accredited through the Higher Learning Commission, North Central Association of Colleges and Schools (NCA). The Mission of Clarkson College is to prepare students to professionally provide high quality, ethical and compassionate health care services. Clarkson College is an educational partner with Nebraska Medicine.
Community Hospital-Fairfax Receives Quality-Based Accreditation from DNV
[Fairfax, MO, 2/9/2024] — Community Hospital-Fairfax announces the successful completion of its new accreditation process from has been awarded by DNV.
By earning accreditation, Community Hospital-Fairfax has demonstrated it meets or exceeds patient safety standards (Conditions of Participation) set forth by the U.S. Centers for Medicare and Medicaid Services. DNV’s accreditation program is the only one to integrate the ISO 9001 Quality Management System with the Medicare Conditions of Participation.
“The DNV program is consistent with our long-term commitment to quality and patient safety,” says Julie Jones, CEO. “The ability to integrate ISO 9001 quality standards with our clinical and financial processes is a major step forward.”
Community Hospital-Fairfax has three years from the date of its accreditation to achieve compliance with ISO 9001, the world’s most trusted quality management system used by performance-driven organizations around the world to advance their quality and sustainability objectives.
“We have taken an entirely different approach to accreditation, and hospitals are really responding,” says DNV Healthcare USA Inc. President Kelly Proctor. “Since accreditation is a must-have credential for just about every hospital in this country, why not make it more valuable, and get more out of it? That’s where ISO 9001 comes into play and turns the typical get-your-ticket-punched accreditation exercise into a quality transformation.”
DNV’s accreditation program, called NIAHO® (Integrated Accreditation of Healthcare Organizations), involves annual hospital surveys – instead of every three years – and encourages hospitals to openly share information across departments and to discover improvements in clinical workflows and safety protocols.
About Community Hospital-Fairfax
Community Hospital-Fairfax is critical access hospital located in Northwest Missouri. Community Hospital-Fairfax provides care through six primary care clinics and a full range of ancillary, inpatient, rehab, and diagnostic services. Learn more about Community Hospital-Fairfax at www.FairfaxMed.com
About DNV
DNV is a global independent certification, assurance and risk management provider, operating in more than 100 countries. Through its broad experience and deep expertise, DNV advances safety and sustainable performance, sets industry benchmarks, drives innovative solutions.
Whether certifying a company’s management system or products, accrediting hospitals, providing training, assessing supply chains or digital assets, DNV enables customers and stakeholders to make critical decisions with confidence, continually improve and realize long-term strategic goals sustainably.
DNV draws on its wide technical and industry expertise to help companies worldwide build consumer and stakeholder trust. Driven by its purpose, to safeguard life, property, and the environment, DNV helps tackle the challenges and global transformations facing its customers and the world today and is a trusted voice for many of the world’s most successful and forward-thinking companies.
For more information about DNV, visit www.dnvcert.com/healthcare
Mina Massey M.D. Joins Community Hospital-Fairfax

Community Hospital-Fairfax Announces Addition of New Family Practice Physician, Mina Massey M.D.
Community Hospital-Fairfax (CH-F) is proud to announce the addition of Mina Massey M.D. to the CH-F Medical Staff. Dr. Massey practiced medicine in southeast Missouri prior to joining CH-F and is passionate about rural medicine.
“When I saw this opportunity, I felt like it was a great fit for my experience and my passions. I wanted to be a part of an organization that is independently owned and has longevity in the community, and I enjoy rural medicine. Community Hospital-Fairfax met both of those objectives,” explained Dr. Massey.
Dr. Massey attended medical school at the University of Missouri-Kansas City and completed her residency at Southern Illinois University School of Medicine. Dr. Massey has provided care in a variety of settings throughout her career including primary care, urgent, obstetrical, and emergency room settings. At CH-F, Dr. Massey will be providing family practice services primarily in the Tarkio Family Medicine Clinic.
“Dr. Massey and I graduated from UMKC School of Medicine in the same class, so it has been great to reconnect. She has a lot in common with our practice style here at CH-F, and we believe that she is a great addition to our team that provides care here in Northwest Missouri,” commented Aron Burke M.D., CH-F Chief Medical Officer.
Dr. Massey’s first day at CH-F was August 14. She is currently orienting to the community and the organization and appointment availability will begin August 31, 2023, at Tarkio. Interested individuals are encouraged to watch local newspapers, CH-F social media and website (www.FairfaxMed.com) for information to schedule appointments with Dr. Massey.
Community Hospital-Fairfax Adds Physician, More Provider Days in Holt County Clinics
Community Hospital-Fairfax is excited to announce the addition of Mina Massey M.D. to the Community Hospital-Fairfax Medical Staff. Dr. Massey will join the Holt County primary care team one day a week in the South Holt Clinic beginning in October. This will increase provider days in Holt County to five days a week in both the Oregon and Mound City clinics.
Community Hospital-Fairfax is excited to offer primary care services in both the Mound City and South Holt Family Medicine Clinics five days a week. Dustin Carpenter M.D. will continue seeing patients at Mound City Family Medicine with Melissa Masonbrink, Family Nurse Practitioner, and Joanna Burke, Pediatric Nurse Practitioner. Dr. Massey will see patients in the South Holt clinic on Wednesdays while Amanda Auxier, Family Nurse Practitioner, takes appointments on Monday, Tuesday, Thursday, and Friday.
“We opened a clinic in Mound City in 2014 and joined the Oregon community in 2016. For nearly 10 years, we have enjoyed tremendous community support. Dr. Massey is looking forward to getting to know the community joining Dr. Carpenter, Melissa, Joanna, and Amanda as part of the Holt County team” commented Julie Jones, CEO.
Dr. Massey attended medical school at the University of Missouri-Kansas City and completed her residency at Southern Illinois University School of Medicine. Dr. Massey has provided care in a variety of settings throughout her career including primary care, urgent, obstetrical, and emergency room settings.
“When I saw this opportunity, I felt like it was a great fit for my experience and my passions. I wanted to be a part of an organization that is independently owned and has longevity in the community, and I enjoy rural medicine. Community Hospital-Fairfax met both of those objectives,” explained Dr. Massey.
Provider information and schedules are available on the hospital website at www.FairfaxMed.com Mound City Family Medicine is located at 514 State Street, Mound City, and can be reached at (660) 442-3181. South Holt Family Medicine is located at 101 S. Washington Street, Oregon, and can be reached at (660) 446-2090
Community Hospital-Fairfax Among Top Hospitals in the Nation for Patient Experience

Becker’s Hospital Review has recently recognized Community Hospital-Fairfax as one of 277, among 5,000 hospitals in the nation, to be rated five stars for patient experience.
The Centers for Medicare and Medicaid (CMS) measures patient experience in ten areas including nurse and physician communication, care transitions, and cleanliness. CMS takes an average of these scores to determine the five-star summary rating. Only seven hospitals in the State of Missouri and 277 hospitals nationwide were given five stars for patient experience in the July 26, 2023, data update.
In addition to this distinction, Community Hospital-Fairfax’s nursing staff was also recognized as a top performer in the nation for responsiveness. The staff responsiveness score is based on patient feedback about how quickly staff responded when the patient asked for help or pressed the call button.
“Providing a quality patient experience has long been a focus of ours at Community Hospital-Fairfax. We constantly review the feedback our patients provide and work to improve to better meet their needs. It is wonderful to see our team recognized for their efforts, commented Samantha Grist, Chief Nursing Officer, and patient experience leader.
All patient survey data is publicly reported on CMS’s Care Compare website at www.Medicare.Gov/Care-Compare Patient experience data for hospitals, long-term care facilities, and many other healthcare providers is available for patients to view on this website.
For more information about Community Hospital-Fairfax, visit www.FairfaxMed.com
May is Mental Health Awareness Month
May is Mental Health Awareness Month, and Community Hospital-Fairfax’s Senior Life Solutions is spreading awareness of the challenges of receiving mental health access in rural areas. While mental illnesses have a similar prevalence in both rural and urban environments, the circumstances and access to treatment look different. The National Rural Health Association (NRHA) tells us that rural residents face more obstacles in obtaining behavioral health services. As a result, distinct mental health differences are seen rurally compared to urban residents.
Studies have also shown that the risk of suicide is higher in rural areas, making it that much more vital that individuals seek out and have access to help. The Rural Health Information Hub states, “suicide rate is near twice as great in the most rural areas of the U.S. compared to the most urban areas.”
Figuring out a solution starts with identifying the problem. The Substance Abuse and Mental Health Services Administration (SAMHSA)highlights the following barriers to receiving mental health care in rural areas:
- Lack of Privacy – “Individuals living in rural locations commonly identify a lack of privacy as a barrier to receiving treatment.
- Lack of culturally appropriate treatment – “Culturally appropriate treatment accommodates clients’ beliefs and practices, preferred languages, individual and family histories, differences in symptoms, and preferred approaches to treatment.”
- Lack of Services – “Even when individuals living in rural locations want treatment, they may have few services and providers in their areas, and they may have less access than urban residents to evidence-based practices (EBPs).”
- Lack of Practitioners – “Rural areas have few behavioral health practitioners, particularly ones who are qualified to provide specialty treatment or EBPs. More than 75 percent of all U.S. counties are mental health shortage areas, and half of all U.S. counties have no mental health professionals at all.”
- Evidence-Based Practices – “Some research shows that behavioral health facilities in rural areas are more likely than their urban counterparts to be independently operated and less likely to collaborate with a university to train providers on EBPs. At the same time, most studies that support EBPs are not conducted in rural areas or on rural populations.”
Recently, amazing solutions such as telehealth have helped increase access to mental health care for rural Americans, making treatment more obtainable. Along with these incredible technological advances, one thing we can all do to help improve access to mental health is simply talking about it. Talking about mental health can open up the door for people to feel more comfortable and less afraid to seek help.
The American Psychiatric Association says, “Research shows that knowing or having contact with someone with mental illness is one of the best ways to reduce stigma. Individuals speaking out and sharing their stories can have a positive impact. When we know someone with mental illness, it becomes less scary and more real and relatable.”
To learn more about how you can become an advocate this Mental Health Awareness Month and join the National campaign,” visit www.nami.org.
Senior Life Solutions is Community Hospital-Fairfax’s ’s program, designed to meet the unique needs of individuals typically 65 and older experiencing depression and/or anxiety related to life changes that are often associated with aging. If you or someone you know is struggling with a recent diagnosis that is difficult to accept or a decline in emotional health, our program wants you to know we are here to help. Whether through our program, or another service, our team works to identify and address the emotional needs of those in our community and provide support.
If you need more information, education, or would like to discuss support, please call (660) 686 2319 or visit www.fairfaxmed.com.
Community Hospital-Fairfax Recognized as a Missouri AIM Star by Missouri Alliance for Innovation on Maternal Health
JEFFERSON CITY, Mo. — Community Hospital-Fairfax was recognized as a Missouri AIM Star by the Missouri Alliance for Innovation on Maternal Health. The recognition signifies the hospital’s completion of the organization’s Severe Hypertension in Pregnancy Collaborative. Hypertension, known as high blood pressure, can have a devastating effect on a mother and baby. Preeclampsia, a condition signaled by high blood pressure, is the leading cause of maternal mortality — occurring in one in every 25 pregnancies.
The MO AIM initiative launched in 2019 to support hospitals’ implementation of evidence-based practices to improve the rapid treatment of high blood pressure and ensure timely follow-up care after delivery. Hospitals within the collaborative participated in education and training, policy development, and data reporting, while increasing patient and family education on the reportable signs and symptoms of high blood pressure in pregnancy.
“The evidence is clear — early intervention for hypertension can save the lives of a mother and child,” said Jon D. Doolittle, Missouri Hospital Association President and CEO. “AIM’s Severe Hypertension in Pregnancy Collaborative is a powerful tool in efforts to reduce maternal and child harm in Missouri. These hospitals are making a difference for their patients.”
“Our obstetrical nursing team along with Aron Burke M.D. has worked diligently to meet the objectives of this program including educating our patients about hypertension and its impact on both the mother and baby’s health. We are grateful for their ongoing commitment to safe, high quality obstetrical care” explained Chief Nursing Officer, Samantha Grist, RN.
During the two-year program, 25 hospitals met the criteria for successful implementation.
Amanda Auxier FNP Joins Community Hospital-Fairfax Family Medicine Clinic at South Holt Clinic
Community Hospital-Fairfax is pleased to announce that Amanda Auxier FNP will be joining our South Holt Family Medicine clinic February 2, 2022. Amanda is the new full-time nurse practitioner in Oregon.
Amanda is a lifelong Northwest Missouri resident and makes her home in rural Savannah. She was a registered nurse for 22 years in a wide variety of healthcare settings before becoming a family nurse practitioner. Amanda has been working in both the Mound City and South Holt clinics over the last few weeks getting to know the clinics and community and is looking forward to her first day at South Holt Family Medicine Clinic on February 2. With Amanda’s arrival, the clinic will now be open four days a week including Monday, Wednesday, Thursday, and Friday.
Rural healthcare is a passion of Amanda’s. She enjoys providing inclusive care to her patients and getting to know multiple generations in a community.
“I’ve worked in rural healthcare for many years and understand its unique nature. I feel very strongly about providing compassionate, cost effective and wholistic care and I can’t wait to get started serving this community” explained Amanda.
When she is not at the clinic, Amanda enjoys fishing and camping with her husband of 21 years, Noel. Together, they have three children and two grandchildren.
Amanda will be the full-time provider in the South Holt Clinic. She joins Dustin Carpenter M.D., Melissa Masonbrink FNP and Joanna Burke PNP, providers in the Mound City Family Medicine Clinic, in serving Holt County and the surrounding areas.
Please reach out to South Holt Family Medicine at (660) 446-2090 for more information.
